Engaging the Vagus Nerve in the Fight Against Lyme Disease and Other Infectious Illnesses
National Lyme Disease Awareness Month is just around the corner (May), providing us with the opportunity and inspiration to reveal more about what we know about this mysterious, persistent, and often debilitating illness.
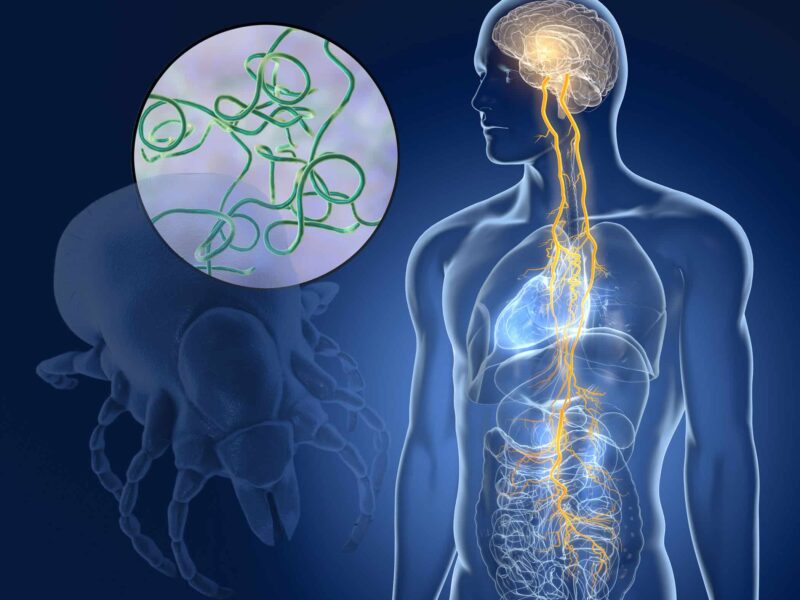
As you may already know, Lyme disease is transmitted by bites from ticks that carry a species of bacteria called bacterium Borrelia burgdorferi or (rarely) Borrelia mayonii. So, it should come as no surprise that the first-line treatment for Lyme disease involves the use of antibiotics over the course of several weeks. That’s the conventional approach, it sometimes works, and it makes sense — at least at first glance.
Unfortunately, blasting away at the bacteria with antibiotics isn’t always enough, and may cause or contribute to the onset of long-term Lyme symptoms, such as the following:
- Headache
- Fever
- Chills
- Fatigue
- Muscle and joint aches
- Facial palsy (loss of muscle tone or droop on one or both sides of the face)
- Arthritis with severe joint pain and swelling, particularly the knees and other large joints
- Intermittent pain in tendons, muscles, joints, and bones
- Heart palpitations or irregular heartbeat
- Episodes of dizziness or shortness of breath
- Inflammation of the brain and spinal cord
- Nerve pain
- Shooting pains, numbness, or tingling in the hands or feet
- Digestive and bowel disorders
Here at Restoration Healthcare, we use a combination of treatments, including prescription antibiotics when called for, in order to eradicate the bacteria, and also strengthen the body’s immune system, dial down the inflammatory response, and restore overall health and vitality.
The truth is that bacterial infection is only the beginning of Lyme disease. Over time, it can become much more complex, involving multiple systems of the body, including the nervous and digestive systems. A functional, integrative approach is often required to eliminate the infection and restore health. This approach often involves toning the vagus nerve.
What Is the Vagus Nerve?
The vagus nerve, also known as the 10th cranial nerve (CN X) is a long nerve that runs from the brain stem, down through the neck, and into the chest and abdomen. The word “vagus” comes from the Latin word for “wandering,” which is a good description in how these nerve fibers connect the brain to the lungs, heart, spleen, liver, kidneys, pancreas, bladder, lymph nodes, and gastrointestinal lining.
You have two of these nerves, one running down either side of your neck. They originate in a part of the brain responsible for autonomic function — regulating vital bodily functions, such as breathing, heartbeat, digestion, and blood pressure — all without your having to direct them consciously. The vagus nerve is primarily responsible for the following:
- Providing sensory input to the throat, lungs, heart, and digestive tract
- Triggering tear and saliva production
- Communicating the sense of taste toward the back of the mouth
- Communicating muscle movement from the brain to neck muscles for speech and swallowing
- Differentiating the air going down the trachea from the food and water going down the esophagus
- Regulating sphincter tone at the top and bottom of the stomach, acid release into the stomach, and bile release from the liver to the gallbladder to the stomach to help digest fats
- Modulating immune system response
- Influencing mood
- Helping to regulate the autonomic nervous system (ANS)
The Doctor Recommends: Learn more about the vagus nerve by reading Restoring Health Through the Vagus Nerve — Using Brain Science to Accelerate Healing here on the Restoration Healthcare blog.
The Sympathetic and Parasympathetic Nervous System
The autonomic nervous system (ANS) consists of two branches, or subsystems, including one that generally acts as the accelerator and the other as the brake:
- Sympathetic autonomic nervous system (SANS) acts as the accelerator (fight or flight), controlling your body’s response to stressful situations. It is always active to a certain degree, but activity elevates significantly in stressful situations through the upregulation of hormone release.
- Parasympathetic autonomous nervous system (PANS) functions as the brake (rest and digest), controlling your body’s response to relaxation, recovery, digestion, and sexual response. It is continuously active to a certain degree, but activity increases shortly after eating and around bedtime. PANS slows the heart rate, dilates (expands) blood vessels, controls muscle movement, and influences memory.
The sympathetic nervous system is primarily activated through the hypothalamic-pituitary-adrenal (HPA) axis, which acts as the accelerator. The vagus nerve is more responsible for stimulating the parasympathetic nervous system, which dials down the stress response and enables the body to heal and recover from illness and other stressful events.
Ideally, the two branches of the ANS accelerate and decelerate other systems in the body to maintain a healthy balance. Imbalances between the two branches impair the body’s regulatory and restorative capabilities.
What causes SANS/PANS imbalances is often a major traumatic event (serious illness or emotional/psychological trauma) or the buildup of less traumatic physical and emotional/psychological stressors over time. These stressors keep the SANS fight-or-flight response in overdrive, making you feel tired, wired, and anxious. At the same time, the PANS rest-and-digest activity is put on hold, impairing the body’s ability to rest and recover.
Short-term imbalances between SANS and PANS function can cause problems, such as these:
- High levels of cortisol result in cell damage and inflammation.
- Tissue and cell growth are negatively impacted.
- Hormone disruption/imbalance occurs, possibly impacting sex hormones, thyroid, and metabolism.
- The liver’s ability to detox is impaired, adding to the body’s toxic burden.
- Digestion is impaired, contributing to nutrient deficiencies and imbalances.
- Neurotransmitters are not released as they should be, adding to anxiety, depression, difficulty sleeping, and more.
Over time, autonomic nervous system dysfunction can develop into chronic conditions with one or more of the following symptoms:
- Chronic fatigue
- Chronic pain, such as fibromyalgia
- Difficulty falling asleep or staying asleep
- Difficulty urinating, incontinence, or incomplete emptying of the bladder
- Difficulty with memory and brain function in the morning
- Dizziness and fainting upon standing
- Erectile dysfunction, vaginal dryness, or difficulty having an orgasm
- Exercise intolerance
- Gastrointestinal/digestive dysfunction (acid reflux, constipation, diarrhea)
- Hormonal/menopause-like symptoms, especially ages 35–45
- Inability to alter heart rate with exercise
- Loss of appetite or difficulty swallowing
- Mood irregularities such as depression, anxiety, panic attacks
- Morning migraines or headaches
- Muscle weakness or tremors
- Sweating too much or not enough
- Vision problems, including blurry vision, or inability to respond to changes in light
Signaling When We Are Sick
In addition to its role in enabling rest and recovery, the vagus nerve provides a two-way communication pathway between the brain and several vital organs:
- 20 percent of your vagus nerve fibers carry signals from your brain to various parts of your body (efferent communication).
- 80 percent of your vagus nerve fibers carry signals to your brain from various parts of your body (afferent communication).
When a potentially harmful virus, bacteria, or parasite threatens the body, the body’s mast cells, and glial cells, release chemicals (cytokines and inflammatory compounds) that trigger an immune response. Sensing this change in the body’s internal environment, the vagus nerve signals the brain, often resulting in flu-like symptoms, such as these:
- Headache
- Fever
- Fatigue
- Joint/muscle pain
- Nausea/vomiting
- Loss of appetite
Together, these symptoms send a strong message that we need to rest, so that the body can direct more of its energy and resources to fighting the infection and recovering. If we ignore the message and push forward, we block the key healing mechanism of the body while continuing to subject it to more stress.
Exploring the Gut-Brain Axis and Its Role in Chronic Illness
The vagus nerve is also a key component of the gut-brain axis — the bidirectional communication system between the central nervous system and the gastrointestinal tract. We have known for some time that the brain regulates digestion, but we are just beginning to recognize how much influence the digestive system has on the brain.
The community of microorganisms living in the gut (the gut’s microbiome, consisting of bacteria and fungi/yeast) actually influences brain health and function. When this community suffers an imbalance — an overgrowth of a potentially harmful bacteria or yeast, or a decline in beneficial bacteria — it can negatively impact brain health and function.
What often happens with Lyme disease and other infectious illnesses, is that patients are prescribed broad-spectrum antibiotics that kill not only the bacteria that cause the infection but also beneficial bacteria in the gut, leading to dysbiosis (an imbalance in the gut’s microbiome). Northeastern University researchers are currently exploring how imbalances in the gut’s microbiome may contribute to long-term symptoms of Lyme.
What is important to note is that the vagus nerve is an essential component of the gut-brain axis. It is the information superhighway responsible for communications back and forth between the gut and the brain.
A Chain Reaction with Devastating Effects
Lyme disease and other infectious illnesses can spark a chain reaction in your body that impacts multiple systems, especially if you are already stressed or your health is compromised.
A bacterial infection, such as one that causes Lyme disease, will trigger an immune reaction resulting in inflammation. Antibiotics used to treat the infection cause dysbiosis resulting in damage to the thin, semi-permeable gut lining, thereby enabling large chemical molecules that should be contained in the gut to escape into the bloodstream, triggering more immune system activity leading to more inflammation.
Sensing the growing threats, the HPA axis fires up the sympathetic nervous system. You feel wired, tired, and anxious and start losing sleep. Your parasympathetic nervous system fails to engage, so your body cannot rest, repair, and recover as it should. Over time, your vagus nerve loses tone and suffers its own dysfunction.
At this point, you are experiencing much more than a bacterial or viral infection:
- Inflammation, which can impact nearly every part of your body
- Immune system disfunction
- Dysbiosis
- Leaky gut
- HPA axis dysfunction
- Nutritional deficiencies, partially due to your digestive issues
- Poor sleep
- Poor vagal tone
No wonder you feel weak, tired, achy, depressed, and anxious.
Undoing the Damage
Effective treatment for Lyme disease and other infectious illnesses often requires reversing the chain reaction that occurred in order to eliminate the infection and restore health:
- In the case of active infection, use antibiotics (prescription and/or natural) to eliminate the infection
- Repair the gut lining
- Restore healthy balance to the gut microbiome
- Restore immune system health and function
- Reduce inflammation
- Test for and address any nutritional deficiencies
- Improve sleep (quantity and quality)
- Restore vagal tone
Restoring Vagal Tone
One of the often-overlooked elements of many treatment plans for nearly any chronic illness is restoring tone to the vagus nerve. There are a variety of do-it-yourself ways to improve vagal tone, including the following:
- When showering, alternate periods of hot and cold water in 60-second intervals two or three times
- Practice meditation, yoga, tai chi, or qi gong
- Hum, sing, or chant
- Gargle
- Dance
- Laugh and engage in joyful social activities
- Induce your gag reflex
Also important is to dial back the stress, both physical and emotional/psychological. Here are a few suggestions:
- Resolve personal and work-related relationship discord
- Address sources of financial stress
- Avoid stressful news, tv shows, movies, and music… anything that starts to make you feel anxious
- Team up with your treatment providers to diagnose and treat any hidden infections, toxic overload, nutrient or micronutrient deficiencies, dietary issues, existing inflammation, and other issues in order to eliminate signals from your body that trigger a stress response.
Here’s our takeaway message: If you’re not feeling 100 percent, and your current doctors haven’t been able to figure out what’s wrong or offer a solution, consult a functional and integrative medical practitioner for a second opinion. Don’t settle for living with chronic fatigue, chronic pain, brain fog, poor sleep, or any of the other symptoms mentioned in this post. Most patients who live with these symptoms are doing so unnecessarily.
If you’re in or near Irvine, Calif., contact us, because here at Restoration Healthcare, we are fortunate to have one of the leading Lyme specialists serving as our medical director. Dr. Sunny Raleigh. Dr. Raleigh is widely recognized by patients and referring physicians as one of the top Lyme doctors in the country. And in Southern California, no medical team is better prepared to help patients with Lyme disease than the team here at Restoration Healthcare.
————-
Disclaimer: The information in this blog post about engaging the vagus nerve in the fight against Lyme disease and other infectious illnesses is provided for general informational purposes only and may not reflect current medical thinking or practices. No information contained in this post should be construed as medical advice from the medical staff at Restoration Healthcare, Inc., nor is this post intended to be a substitute for medical counsel on any subject matter. No reader of this post should act or refrain from acting on the basis of any information included in, or accessible through, this post without seeking the appropriate medical advice on the particular facts and circumstances at issue from a licensed medical professional in the recipient’s state, country or other appropriate licensing jurisdiction.


